Diabetes Care
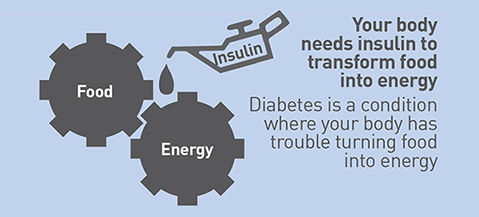
Diabetes is a condition where your body has trouble turning food into energy. Insulin is the key hormone that helps turn food into energy.
There are several different forms of diabetes, but they all involve something going wrong with your insulin production.
Seven million people live with the disease but don’t know they have it. Another 84 million have prediabetes —a reversible condition that can lead to diabetes if you don’t change course.
_________________________________________________________
Diabetes Classes
The more you know about diabetes, the better you can manage it.
Investing now in your education about diabetes and prediabetes can help you prevent serious complications and allow you to live your best life.
Learn more by calling 206.326.2440
_________________________________________________________
Class Description
Diabetes: The Real Deal
Learn survival skills for managing diabetes: how to monitor blood sugar, how to treat highs and lows, and how to help prevent complications. We’ll also go over why medications are prescribed and the basic physiology of diabetes.
The Power of Food
Learn the basic principles of nutrition and how food can help manage diabetes. We’ll review carb counting and label reading as well as healthy food choices and basic meal planning.
_________________________________________________________
Diabetes Classes
2026 Diabetes Education Class Schedule
All classes are in-person this year.
Our diabetes classes each include two 2-hour sessions, instructed by a registered dietitian and certified diabetes educator.
April 8th & 15th | 3:00-5:00pm
Renton: 1801 Lind Ave SW, Building D Renton, WA 98057
May 13th & 20th | 10:00am-12:00pm
Beacon Hill: 1200 12th Ave S, Seattle, WA 98144
June 10th & 17th | 3:00-5:00pm
Canyon Park: 1909 214th St SE, Suite 300, Bothell, WA 98021
September 16th & 23rd | 10:00am-12:00pm
Northgate: 10416 5th Ave NE, Seattle, WA 98125
October 7th & 14th | 3:00-5:00pm
Renton: 1801 Lind Ave SW, Building D Renton, WA 98057
November 4th & 11th | 3:00-5:00pm
Canyon Park: 1909 214th St SE, Suite 300, Bothell, WA 98021
To sign up for a class, please call 206.326.2440 and leave a message. One of our team members will get back to you within the week. You can also reach out to your dietitian or doctor via MyChart to sign up or get more information.
If these classes don’t work for your schedule, our dietitian and/or diabetes educator can see you individually for education.
_________________________________________________________
How diabetes works
Download our Diabetes Introduction packet for an overview to the condition.
 TYPE 1 DIABETES The pancreas doesn’t produce insulin. |
 TYPE 2 DIABETES Insulin is in short supply or doesn’t work as well (also called insulin resistance). |

PREDIABETES |
There are different maintenance schedules for people with diabetes, people with prediabetes, and healthy people who want to prevent diabetes.
If you want to stay on course around diabetes, follow the recommended maintenance schedule to know when to visit your doctor and what to ask for.
For patients with Diabetes:
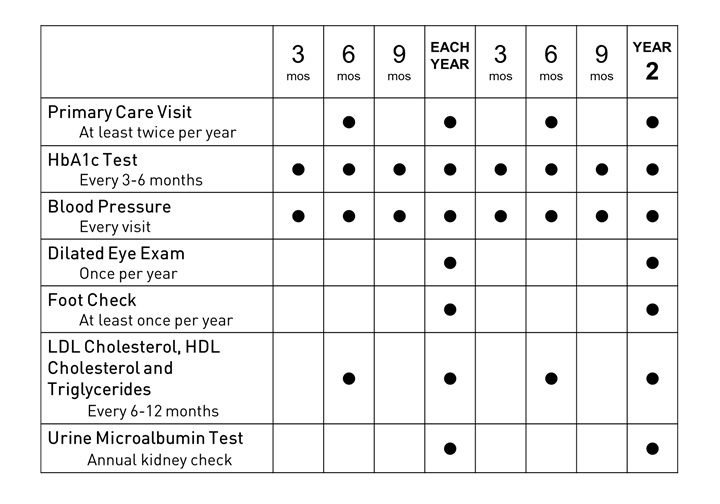
Your diabetes care team will build a personalized relationship with you. They will communicate with you and your
other doctors about diagnostic testing, monitoring and disease treatment.
Connecting with your care team may include doctor visits, telephone check-ins, educational classes and nutritional
planning.
Your diabetes care team includes:
- Primary care: Your primary care provider manages the majority of your day-to-day needs. They are
trained experts who can provide information and who will partner with you to develop a management plan that works
for you. You may have telephone or virtual visits to check in on your progress. - Diabetes specialists:
- Registered dietitians (and certified diabetes educators) who will assist you with healthy
food choices and lifestyle changes, an essential part of living with diabetes successfully. - Clinical pharmacists for medication management and questions about your current medications
- Optometrists and ophthalmologists for regular eye care
- Podiatrists for foot care and preventive checks
- Behavioral therapists to treat depression, which can get in the way of successful self-care.
- Registered dietitians (and certified diabetes educators) who will assist you with healthy
- Other PacMed medical staff members: These include our nurses and medical assistants. These
educators can help you with blood sugar testing, management, coaching, healthy eating choices and much more.
Bring a few things to your diabetes care team visit:
- Your family and friends are an important part of your care team and are invited to join you at
any of your appointments and education sessions. - Your blood sugar levels: We ask that you check and bring your
daily blood sugars to this appointment. If you keep a log—bring it with you. If you keep your blood sugars on a
meter—bring your meter. If you keep track on a computer—bring a printout.- You may have more frequent appointments until your blood sugars return to normal.
- What you eat: We need to know the foods you eat and when you eat them in a typical 24-hour day, including snacks. You can write down everything you eat in a day, take pictures of what you eat on your phone or if you keep track on an app, bring in a sample day.
- What exercise you do: We need to know how often you exercise and for how long.
- What medications you might be on (especially if you are new to PacMed).
Regionally respected diabetes care
At PacMed, we are here to support you through your journey with diabetes—whether that means living with it or preventing it. We’ll be with you every step of the way to care for your diabetes as a team.
- Recognized as a Patient Centered Medical Home™ by the National Committee for Quality Assurance (NCQA). The NCQA has given us a 95-point rating (out of 100) for “consistently providing a high level of diabetes care.”
- Among the best in the Northwest. Any primary care provider at PacMed can help you with diabetes. Many providers have also taken steps to earn recognition by the NCQA, as part of an elite group of professionals who demonstrate the highest possible level of care for their patients with diabetes.
- Accredited. Our diabetes education program, featuring the team below, is accredited by the American Association of Diabetes Educators.






